Cervical cancer is staged from 0 to IV based on tumour size and depth of invasion.
While early stages (I-IIA) are often treated with surgery or targeted radiation, advanced stages (IIB-IV) require a combination of chemotherapy and high-precision radiation therapy to achieve remission.
Cervical cancer- The fear is Evident Nation-Wide
Cervical Cancer -two words can instantly trigger a wave of fear and uncertainty. Yet, understanding this disease, its stages, and the available treatment options is the first crucial step towards empowerment.
If you’re seeking a cervical cancer doctor in Kolkata, this comprehensive guide by Dr Mukti Mukherjee aims to equip you with the knowledge to navigate this challenging journey with clarity and confidence.
Cervical Cancer Explained: How Does it Progress?
Cervical cancer is a type of cancer that begins in the cells of the cervix, the lower part of the uterus that connects to the vagina. It usually develops slowly over time, often starting as precancerous changes called dysplasia, which, if left untreated, can progress into invasive cancer.
Cervical cancer primarily originates from persistent infection with certain high-risk types of Human Papillomavirus (HPV). These viral infections can cause abnormal cell changes on the cervix, leading to precancerous lesions and, eventually, full-blown cancer if not detected and managed early. Understanding the underlying cause is vital for both prevention and effective treatment strategies.
Early Detection of Cervical Cancer – Why is it so crucial
Early detection of cervical cancer is crucial because it significantly improves treatment outcomes and increases the chances of a complete cure. When detected at its initial stages, the cancer is often localised, making it easier to treat effectively.
Imagine finding a small, unwelcome weed in your garden. Pluck it out early, and your garden remains healthy. Let it grow, spread its roots, and it becomes a much bigger, more challenging problem to eradicate.
Key Stages of Cervical Cancer
The key stages of cervical cancer describe how far the cancer has spread, from a very localised tumour to one that has metastasised to distant parts of the body.
These stages are categorised using the FIGO (International Federation of Gynaecology and Obstetrics) system.
Understanding the stages of cervical cancer is fundamental for your medical team to determine the most effective treatment plan. It’s a roadmap that guides decisions, and knowing your stage can help you better understand your prognosis and options.
Here’s a breakdown of the cervical cancer stages:
| Stage | Extent of Disease (At a Glance) |
| 0 | Abnormal cells only on the cervical surface (pre-cancer). |
| I | Cancer is limited to the cervix. IA: Microscopic only (<5 mm depth)IB: Visible or >IA, ≤ cervix (<2 cm → >4 cm). |
| II | Beyond the cervix, not the pelvic wall/lower vagina. IIA: Upper vagina only ( <4 cm / ≥4 cm ) IIB: Parametrial spread. |
| III | Lower vagina, pelvic wall, kidney impact, or nodes. IIIA: Lower vagina. IIIB: Pelvic wall/hydronephrosis. IIIC: Pelvic or para-aortic lymph nodes. |
| IV | Spread outside the pelvis.IVA: Bladder or rectum. IVB: Distant organs (lung, liver). |
Symptoms of Cervical Cancer Linked to Its Stages?
Cervical cancer symptoms stages often progress from subtle to more noticeable as the disease advances, though early stages might be asymptomatic, underscoring the importance of regular screening.
Pap smears and HPV tests are lifesavers
For many women, particularly in the earliest stages, there are no obvious symptoms. This silent progression is why Pap smears and HPV tests are lifesavers.
When symptoms do appear, they can include:
- Abnormal vaginal bleeding: Bleeding between periods, after sex, or after menopause. This is often one of the first and most alarming signs.
- Unusual vaginal discharge: May be watery, bloody, or have a foul odour.
- Pelvic pain or pain during intercourse: As the tumour grows and presses on nearby tissues.
- Difficulty urinating or having bowel movements: If the cancer has spread to the bladder or rectum (later stages).
- Swelling in the legs: If the cancer affects lymph nodes, blocking lymphatic drainage.
If you experience any of these symptoms, do not delay seeking medical advice. It could be something benign, but it needs to be checked. A prompt consultation with Dr Mukti Mukherjee, a cervical cancer doctor in Kolkata, can make all the difference.
Cervical Cancer Testing and Diagnosis Explained

Cervical cancer diagnosis typically involves a combination of screening tests, physical examinations, and more specific diagnostic procedures to confirm the presence of cancer and determine its stage.
The diagnostic journey
| Evaluation Step | Purpose Before Radiation Therapy | What It Involves |
| Pap Test (Papanicolaou Test) | Detects abnormal or precancerous cervical cell changes at an early stage. | Cells are gently collected from the cervix and examined for abnormal or cancerous changes. |
| HPV Testing | Identifies high-risk HPV strains associated with cervical cancer development. | Laboratory testing checks for cancer-causing HPV types, often alongside a Pap test. |
| Colposcopy Examination | Allows detailed visual assessment when screening tests show abnormalities. | A magnifying instrument examines the cervix closely to accurately locate suspicious areas. |
| Biopsy Confirmation | Confirms cancer diagnosis and tumour type before treatment planning. | Small tissue samples are taken from abnormal areas and analysed under a microscope. |
| Imaging for Radiation Planning | Determines tumour size, spread, and exact treatment targeting. | MRI, CT, or PET scans help radiation oncologists plan precise radiation delivery while protecting healthy tissues. |
Core Treatment Approaches for Cervical Cancer
Cervical cancer treatment options vary significantly based on the stage of the cancer, the patient’s age, overall health, and personal preferences, often involving a multidisciplinary approach.
Here’s a look at the main treatment modalities:
1. Early-Stage Cervical Cancer Treatment
Early-stage cervical cancer treatment often aims to remove the cancerous cells while preserving fertility, where possible, focusing on less invasive procedures.
| Treatment Type | Description | Ideal For |
| Cone Biopsy (Conisation) | Removal of a cone-shaped piece of tissue containing the abnormal cells. | Stage 0, IA1, and sometimes IA2, especially if future fertility is desired. |
| LEEP (Loop Electrosurgical Excision Procedure) | Uses a thin, heated wire loop to remove abnormal tissue. | Stage 0, IA1. |
| Hysterectomy | Surgical removal of the uterus and cervix. May also remove surrounding tissues and lymph nodes. | Stage IB1, IB2, IIA1 when fertility preservation is not a concern. |
| Radical Hysterectomy | Removal of the uterus, cervix, part of the vagina, and extensive surrounding tissue and lymph nodes. | Stage IB2, IIA1, or IIA2. |
2. Radiation Therapy for Cervical Cancer
Radiation therapy for cervical cancer uses high-energy X-rays or other particles to kill cancer cells or inhibit their growth, often a cornerstone of treatment for more advanced stages.
Dr Mukti Mukherjee, an experienced cervical cancer doctor in Kolkata, specialises in advanced radiation techniques:
External Beam Radiation Therapy (EBRT)
Radiation is delivered from a machine outside the body. Often combined with chemotherapy.
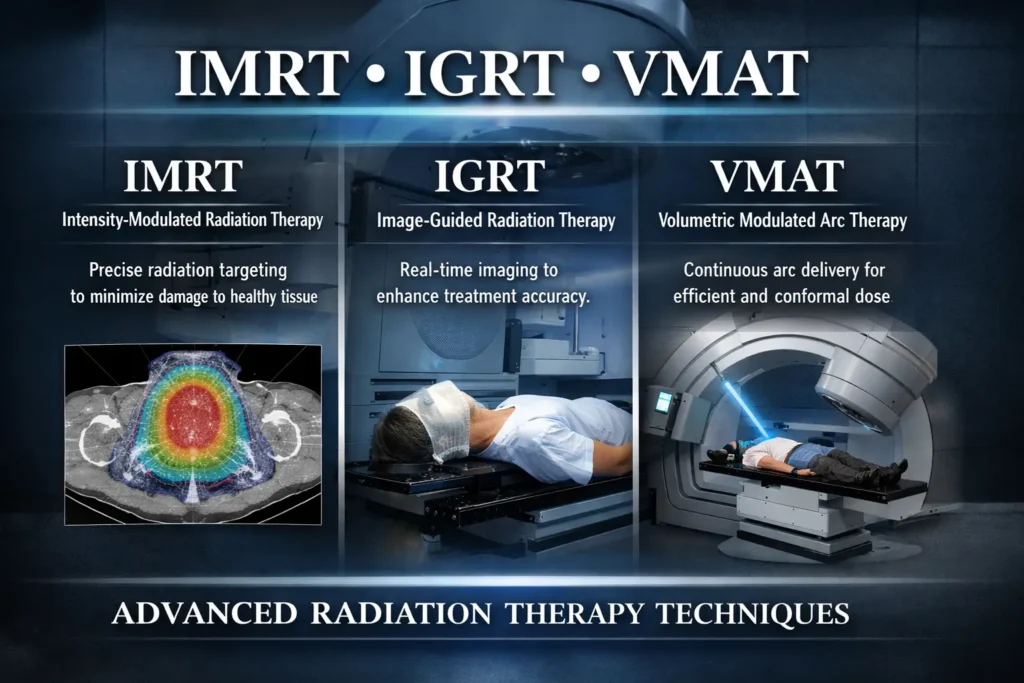
- IMRT (Intensity-Modulated Radiation Therapy): Delivers precise doses of radiation shaped to the tumour, sparing surrounding healthy tissue.
- IGRT (Image-Guided Radiation Therapy): Uses imaging during treatment to ensure accurate tumour targeting.
- VMAT (Volumetric Modulated Arc Therapy): A type of IMRT that delivers radiation in a continuous arc, significantly reducing treatment time.
Brachytherapy (Internal Radiation)
A radioactive source is placed inside or near the tumour.
- Intracavitary Brachytherapy: Applicators are placed in the vagina and/or uterus.
- Interstitial Brachytherapy: Needles are placed directly into the tumour.
| Radiation Type | How it Works | Common Use Case |
| External Beam (EBRT) | The machine outside the body targets the pelvis. | Primary treatment for locally advanced cervical cancer (Stage IIB-IVA), often with chemotherapy (chemoradiation). |
| Brachytherapy | Radioactive source placed directly in/near the cervix/uterus. | Boost dose after EBRT, especially for more localised but advanced disease, or for specific early stages. |
3. Chemotherapy for Cervical Cancer
Chemotherapy for cervical cancer uses drugs, either orally or intravenously, to kill cancer cells throughout the body or to enhance the effects of radiation therapy.
Concurrent Chemoradiation
Chemotherapy is often given concurrently with radiation therapy (chemoradiation) for locally advanced cervical cancer (Stage IIB-IVA). The chemotherapy drugs, typically cisplatin-based, act as “radiosensitisers,” making the cancer cells more susceptible to the effects of radiation.
Systemic Chemotherapy
For metastatic or recurrent cervical cancer (Stage IVB or recurrent disease), chemotherapy might be used alone or in combination with targeted therapy or immunotherapy to control disease spread and manage symptoms.
4. Targeted Therapy & Immunotherapy
These newer treatments are becoming increasingly important for advanced or recurrent cervical cancer:
Targeted Therapy
Drugs that specifically target molecules involved in cancer growth and spread. For example, bevacizumab (Avastin) targets VEGF, a protein that helps tumours form new blood vessels.
Immunotherapy
Helps your body’s immune system fight cancer. Pembrolizumab (Keytruda) is an example, often used for recurrent or metastatic cervical cancer that progresses after chemotherapy.
Act Before the Choice is Taken Away
Cervical cancer is a ruthless opponent, but it is a predictable one. You have the power to stop it, provided you don’t let modesty or fear stand in the way of a check-up.
Whether it is vaccination, regular screening, or seeking a specialist cervical cancer doctor in Kolkata, your actions today determine your presence in the future.
Consult Dr Mukti Mukherjeetoday.
People Also Ask
What is Stage 1 cervical cancer treatment?
Stage 1 cervical cancer is treated with surgery or radiation therapy, offering high cure rates when diagnosed early through regular screening.
What are Stage 1 cervical cancer symptoms?
Early signs may include abnormal bleeding, unusual discharge, pelvic discomfort, or no symptoms, making routine screening essential for early detection.
How is Stage 1B2 cervical cancer treated?
Treatment usually combines surgery with radiation therapy or chemotherapy, based on tumour size, spread risk, fertility goals, and overall patient health.
What is Stage 2 cervical cancer treatment?
Stage 2 cervical cancer is commonly treated with combined radiation therapy and chemotherapy to control tumour spread and improve treatment outcomes.
What is the life expectancy of Stage 2 cervical cancer with treatment?
With timely therapy, many patients achieve favourable survival outcomes, especially when the cancer responds well to radiation treatment and chemotherapy protocols.
What is the life expectancy of Stage 3 cervical cancer with treatment?
Combined radiation therapy and chemotherapy can slow disease progression, improve survival rates, and help maintain comfort and quality of life.